A Hidden Smile - The Pet Dental Health Crisis
- Justin Lim
- 3 days ago
- 5 min read

(Source: bestfriendpetcare)
Doing visual inspections on your pet for obvious physical abnormalities is a must for every pet owner. However, while we often spend our time focusing on the visible markers of our pets health, it is easy to miss and graze over certain things. One of the less noticeable areas are the teeth.
Bad breath in dogs and cats is so commonly dismissed as a quirk of being a pet. That smell is frequently the first detectable sign of a chronic disease that, left unaddressed, can quietly damage a pet's kidneys, heart, and liver long before any outward signs appear.
Dental disease is the most common health condition diagnosed in companion animals, and yet it remains one of the least discussed at home. So lets discuss and breakdown the ins and outs of dental disease and their complications.
How Common Is Dental Disease in Pets?
(Source: PDSA)
The numbers are striking. Data drawn from over three million pet visits in a 2023 research study, found that 73% of dogs and 64% of cats were diagnosed with dental-related issues that year. Separate research estimates that by age three, roughly 80% of dogs and cats have some form of periodontal disease. It is also noted that extra-small dog breeds under 6.5 kilograms were up to five times more likely to be diagnosed with periodontal disease than giant breeds.
Breed size is not the only risk factor however. The same study identified being overweight and a longer gap since the last professional dental cleaning as additional risk factors for disease. Among cat-specific conditions, periodontal disease, tooth resorption, and early-onset gingivitis are among the most frequently encountered oral diseases in domestic cats, many of which go undetected because cats instinctively mask discomfort.
What is Periodontal Disease?

(Source: Fish for dogs)
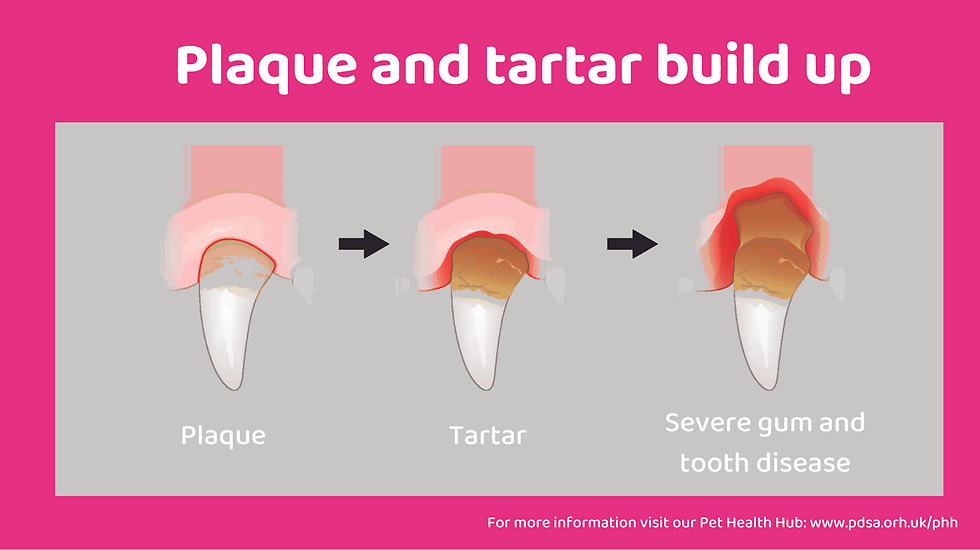
Periodontal disease is an infection of the tissues that support the teeth. It begins with plaque, a soft bacterial biofilm that forms on tooth surfaces. When plaque is not mechanically disrupted through brushing or other means, it mineralizes into tartar within days. Tartar provides a rough surface that accelerates further plaque accumulation, including below the gumline where standard brushing cannot reach.
The first stage, gingivitis, is the inflammation of the gum tissue and is the only stage that is fully reversible with proper treatment and home care. Once the disease progresses to periodontitis, the deeper supporting structures of the tooth begin to break down irreversibly. Periodontal pockets form, bone loss occurs, and teeth become loose. In severe cases, particularly in smaller breeds, jawbone fracture can result from extensive bone loss around the tooth roots.
Because much of this damage occurs below the gumline and pets cannot communicate pain the way humans do, the disease often progresses significantly before an owner notices anything is wrong. Research identified that full dental radiographs reveal more than visual examination alone, and that 27.8% of dogs and 41.7% of cats may have clinically significant lesions that would be missed without intraoral X-rays.
The Impending Health Crisis

(Source: Getty Images)
Dental disease does not stay in the mouth. Bacteria from infected tissues can enter the bloodstream, a process known as bacteremia. In healthy animals, the immune system typically clears these bacteria quickly. But in pets with advancing periodontal disease, chronic bacteremia and the inflammatory mediators it generates can place ongoing stress on distant organs.
Prior research found that there is a strong association between periodontal disease and cardiac disease. Another study found that the hazard ratio for developing azotemic chronic kidney disease increased with each advancing stage of periodontal disease, reaching a hazard ratio of 2.8 at the most severe stages.
It is worth being precise here: the relationship between periodontal disease and systemic organ disease in pets is one of association, not definitively proven causation in all cases. What the evidence does support is that chronic oral infection and inflammation represent a meaningful risk factor for organ health, particularly in older pets and those with pre-existing conditions.
Home Care

(Source: Ourvets Parklands Veterinary Clinic)
Tooth brushing remains the gold standard. Research demonstrated that brushing daily or every other day produced statistically significant reductions in plaque and tartar scores. The mechanical action of the bristles on tooth surfaces is what matters, and the Veterinary Oral Health Council (VOHC) recommends focusing particular attention on the cheek-facing surfaces of the upper teeth, where plaque and tartar accumulate most rapidly.
For pet owners who cannot achieve daily brushing, VOHC-accepted alternatives exist. These include dental diets (such as Hill's Prescription Diet t/d, which uses a fibrous kibble matrix designed to mechanically clean the tooth surface as the pet chews), dental chews (including several sizes of Greenies and Virbac C.E.T. Oral Hygiene Chews), water additives, and topical wipes. Each of these carries a lower efficacy ceiling than brushing but provides measurable benefit still.
One important caveat on dental chews: size matters. The VOHC explicitly advises that chews be matched to the appropriate body weight of the dog, and that owners should observe their pet during chewing to reduce the risk of gastrointestinal obstruction from large pieces being swallowed. This is particularly relevant for dogs who eat quickly.
For toothpaste, it is important to note that human toothpaste should never be used on pets. Many contain xylitol, which is toxic to dogs, and fluoride concentrations that are harmful when swallowed. Only pet-specific toothpastes should be used, and where possible.
The Role of Professional Dental Cleanings

(Source: Papaya Veterinary Care)
Home care cannot replace professional cleanings, and professional cleanings cannot replace home care. They serve different functions and work best in combination. A professional cleaning session must be performed under general anesthesia. This is non-negotiable for a thorough evaluation, as without anesthesia, necessary procedures cannot be safely or accurately performed.
Anesthesia-free dental cleanings, which are offered at some grooming facilities and pet stores, remove visible tartar from crown surfaces but do not address the subgingival disease where the real damage occurs. They also carry their own risks, including stress and aspiration, without delivering the diagnostic value of a proper examination. The American Veterinary Dental College (AVDC) and the American Animal Hospital Association (AAHA) both discourage anesthesia-free dental procedures, so do note that if you are considering a session.
Most dogs and cats should have a professional dental evaluation every six to twelve months, with frequency depending on age, breed, and individual risk profile. Smaller breeds and older pets generally benefit from more frequent monitoring.
Signs That Should Prompt a Veterinary Visit

(Source: Morgan Pet Clinic)
Because dental pain is frequently masked, particularly in cats, many owners do not recognize it until the disease is well advanced. There are, however, observable indicators. Persistent chronic bad breath that does not resolve after a few days of brushing is one of the most consistent early signs. Visible red or swollen gum tissue along the gumline, brown or yellow deposits on the teeth, and changes in eating behavior such as dropping food, chewing on one side, or a sudden reluctance to eat hard food should all prompt an oral examination.
In cats, the 2025 FelineVMA guidelines note that clinical signs can also include facial rubbing, pawing at the mouth, and reduced grooming, though these are not always present. Cats in particular may continue to eat despite significant oral pain, driven by survival instinct, so the absence of obvious appetite changes should not be interpreted as an absence of discomfort.
The most practical takeaway from the research is also the simplest: start early, and be consistent. Introducing toothbrushing during kittenhood or puppyhood, before disease has established itself, is significantly effective. Combining home care with regular professional evaluations is the approach most strongly supported by veterinary dental evidence. These things require commitment, and the difference in long-term outcomes, for teeth and for the organs that depend on a healthy immune system, is meaningful.
So do keep an eye out for your little ones, may they may live long and healthy!
References and helpful links




Comments